
Alera Care Medical
Alera Care Medical

Alera Care delivers premium, hospital-grade specialty infusion services designed to support patients with complex autoimmune, inflammatory, neurologic, immunologic, dermatologic, and anemia-related conditions. We provide Specialty Infusion Services across rheumatology (RA, lupus, vasculitis), gastrointestinal care (Crohn’s, UC), neurology infusions (MS and neuro-autoimmune), immunology infusions (IVIG), dermatology infusion support (autoimmune biologics), and iron infusions with anemia management.
Our care model is built for physician trust and payer credibility, focused on safe infusion protocols, attentive clinical monitoring, and streamlined coordination with referring providers to keep patients on schedule. We treat a broad range of conditions, including rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, lupus, vasculitis, Crohn’s disease, ulcerative colitis/IBD, multiple sclerosis, NMO, myasthenia gravis, CIDP, immune deficiency disorders, psoriasis, and iron deficiency anemia.
At Alera Care, we combine clinical precision, coordinated care, and a calm, supportive environment, so patients and families feel confident, comfortable, and cared for at every visit.
Care We Provide
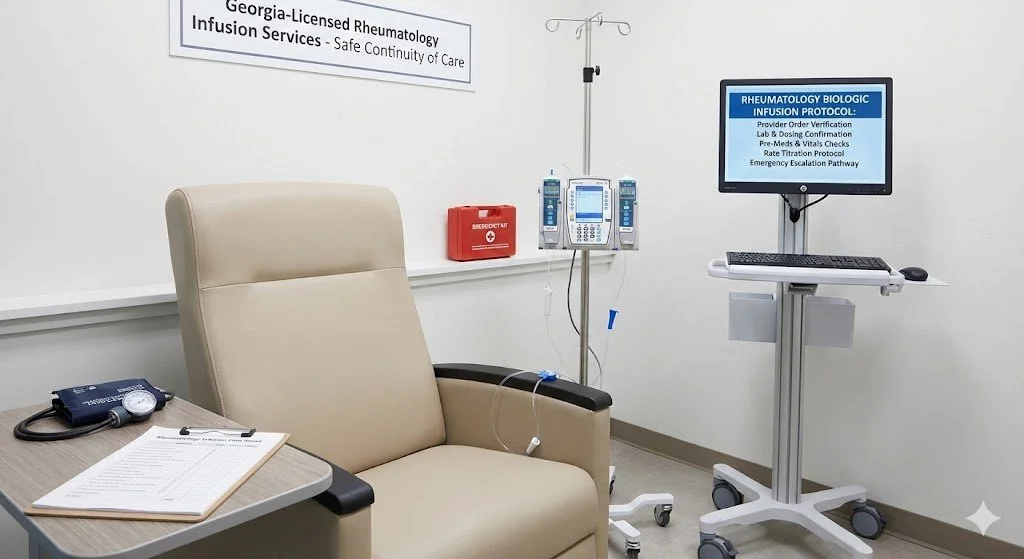
Rheumatology Infusion Therapy (RA, lupus, vasculitis)
Our Georgia-licensed infusion nurses deliver rheumatology biologic infusions strictly per provider orders—screening history, verifying labs, confirming dosing, and administering pre-meds as indicated. We perform baseline and interval vital checks, titrate infusion rates per protocol, and respond to reactions with a defined escalation pathway and emergency readiness (supplies, meds, and transfer procedures). We coordinate updates with rheumatology teams to support safe continuity of care.
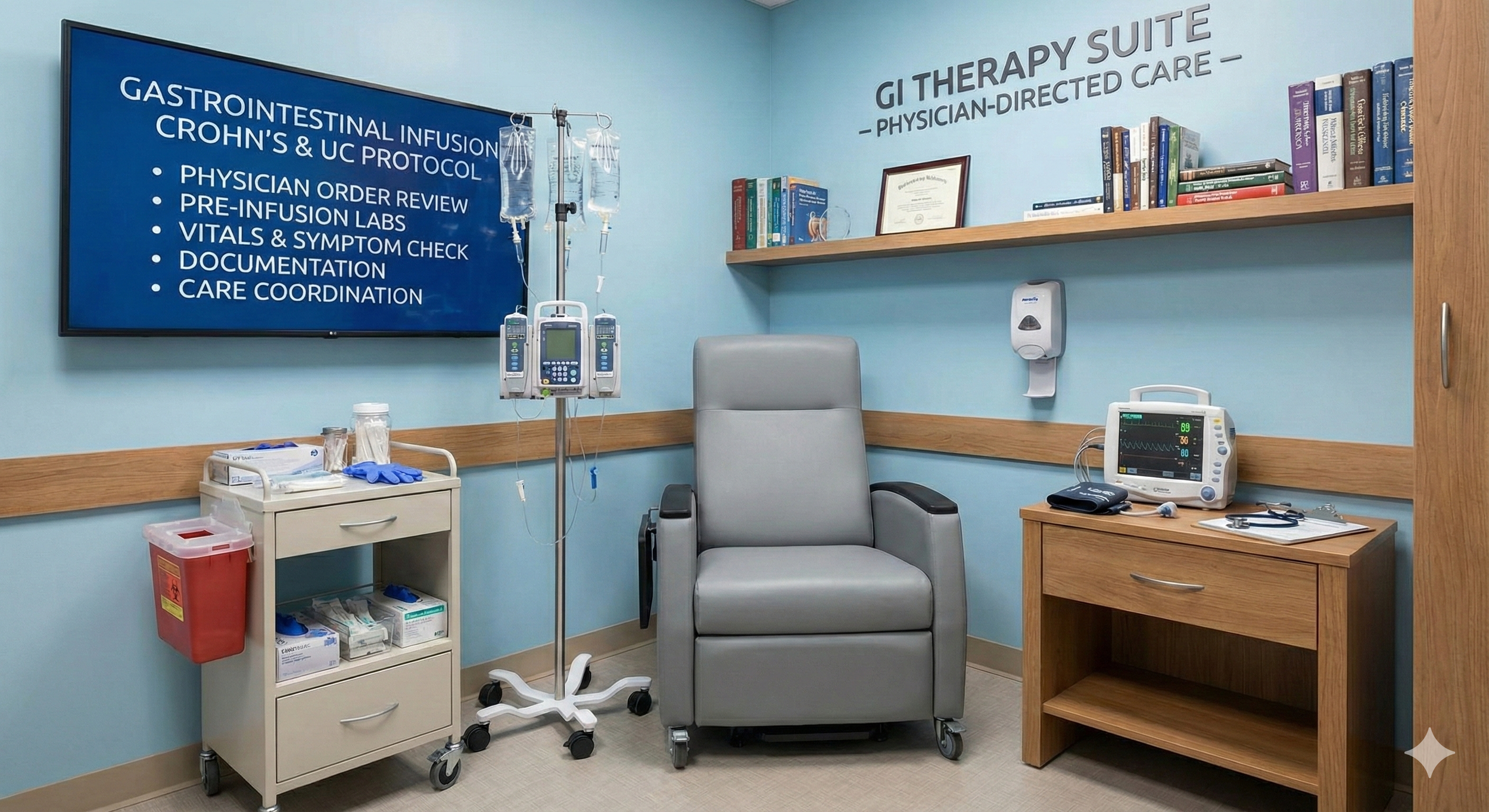
Gastrointestinal Infusion Therapy (Crohn’s, UC)
Our GI infusion workflow follows physician-directed protocols for IBD therapies—ensuring referral accuracy, required screenings/labs, medication verification, and patient education before each visit. Nurses monitor vitals, comfort, and symptoms throughout treatment, document response, and manage infusion reactions using standardized steps. We coordinate with gastroenterology offices for ongoing plan adjustments, missed-dose recovery, and timely clinical reporting to keep patients stable and consistent with therapy.
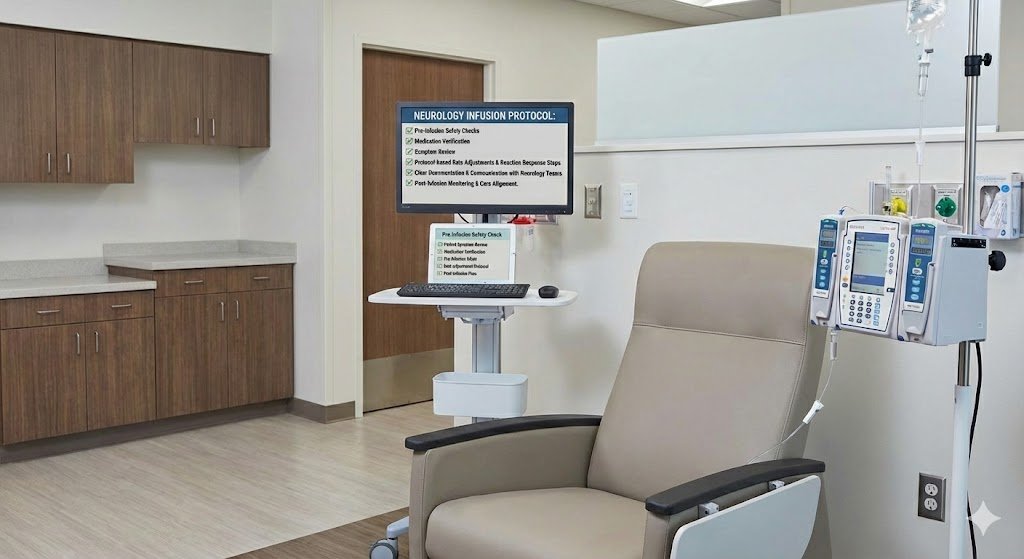
Neurology Infusions (MS and neuro-autoimmune)
We provide neurologic infusion support under neurologist orders with careful pre-infusion safety checks, medication verification, and symptom review. Our team monitors vitals, infusion tolerance, and neuro-relevant concerns during and after therapy, using protocol-based rate adjustments and reaction response steps. We maintain clear documentation and communicate outcomes to neurology teams to support adherence, reduce treatment disruption, and keep care aligned across visits.
Immunology Infusions (IVIG)
Our IVIG process is built around precise verification and safety: weight-based dosing confirmation, infusion rate titration per protocol, hydration/premed support as ordered, and close monitoring for tolerance. Nurses document vitals and patient response at scheduled intervals and follow an escalation pathway for adverse reactions. We coordinate with immunology teams on lab requirements, scheduling cadence, and post-infusion notes to support consistent immune therapy management.
Dermatology Infusion Support (autoimmune biologics)
We support systemic biologic therapy for autoimmune dermatologic conditions through a clinic-based infusion workflow grounded in provider orders and standardized monitoring. Each visit includes medication verification, screening checklist review, and vitals monitoring with protocol-driven rate management. Our team documents treatment response and side effects, then shares structured updates with dermatology offices to keep therapy on track while maintaining a calm, patient-first infusion environment.
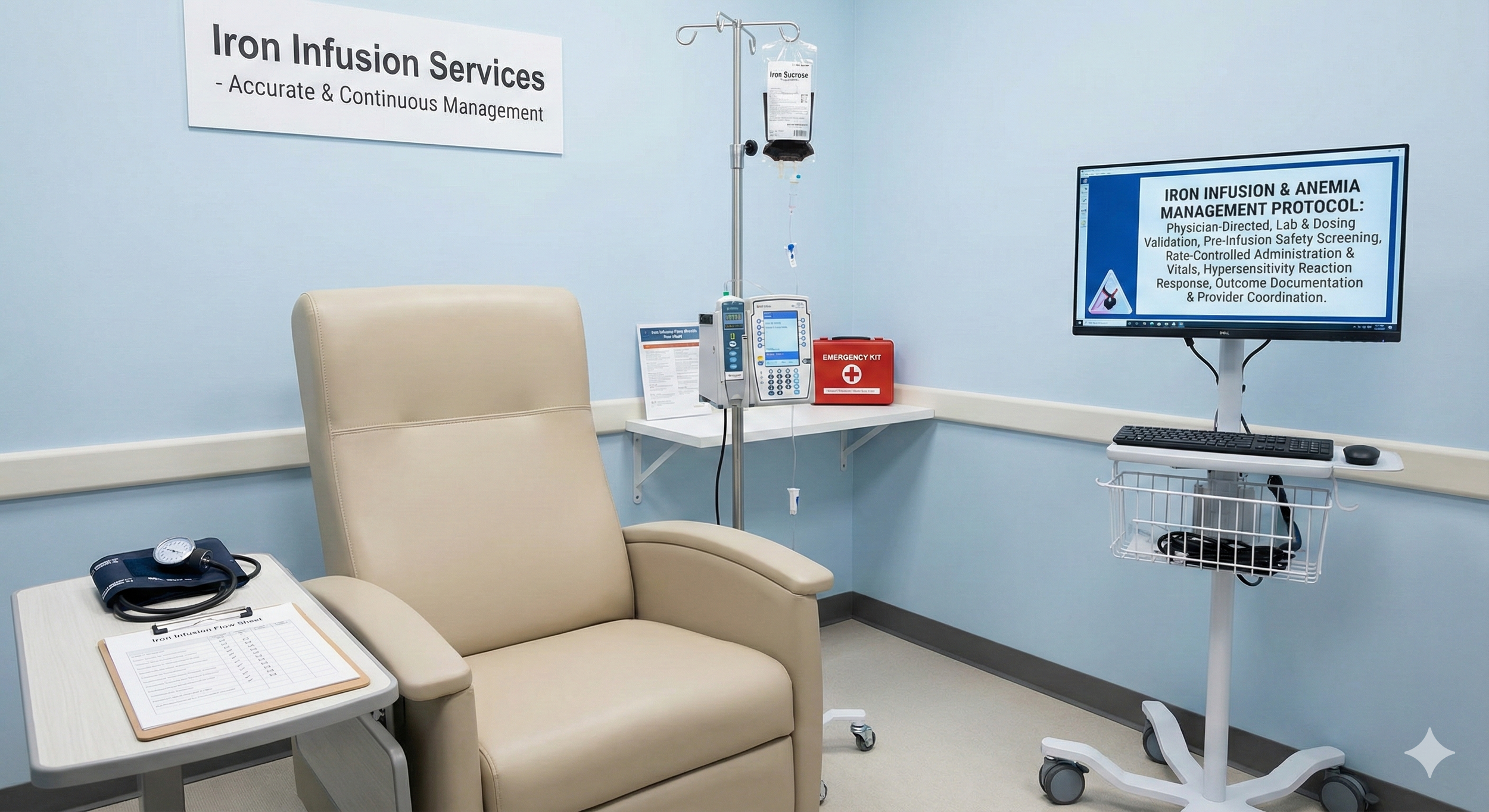
Iron Infusions & Anemia Management
A practical, room-by-room approach to reduce avoidable injuries and keep aging adults confident at home. We review lighting, rugs/cords, bathrooms, stairs, and transfer points; suggest simple fixes (grab bars, shower chairs, rails, non-slip mats), and coordinate with DME vendors when requested. Caregivers reinforce safe ambulation, gait-belt use, and timed toileting; provide exercise cueing from provider guidance; and build morning/evening routines that lower risk. When ordered/appropriate, nurses monitor vitals/edema and escalate changes promptly—turning safety plans into daily habits.

Oncology Infusion Services
We provide oncology infusion therapy through a carefully controlled workflow guided by oncologist orders, clinical protocols, and specialized safety procedures. Each visit includes medication verification, patient assessment, vitals monitoring, and treatment administration with close observation throughout the infusion process. Our oncology-trained nurses document response, side effects, and tolerance, then coordinate updates with the oncology team to support continuity of care while maintaining a safe, compassionate treatment environment.

Oncology Support Infusion Services
We provide supportive oncology infusion therapies through a structured care model designed to complement active cancer treatment and provider-directed plans. Each visit includes medication verification, symptom review, patient assessment, and vitals monitoring with close observation for tolerance and adverse effects. Our oncology-trained nurses document response and supportive care needs, then share timely updates with the oncology team to help maintain comfort, stability, and continuity throughout treatment.

Allergy & Asthma Biologic Therapy Support
We support allergy and asthma biologic therapy through a structured infusion workflow guided by provider orders and standardized safety monitoring. Each visit includes medication verification, pre-treatment screening, review of relevant clinical information, and vitals monitoring with observation tailored to the ordered therapy. Our nurses document treatment response and adverse reactions, then coordinate updates with allergy, immunology, and pulmonary teams to support continuity of care in a calm, patient-first infusion environment.
Conditions We Treat
-
Diseases/Concerns Supported:
Rheumatoid arthritis
Lupus
Vasculitis
Other autoimmune and inflammatory rheumatologic conditions
Care We Provide:
Rheumatology biologic infusion administration per provider orders
Patient history screening and pre-infusion assessment
Lab verification and dosing confirmation
Pre-medication administration as indicated
Baseline and interval vital signs monitoring
Protocol-based infusion rate titration
Observation for infusion reactions and escalation as needed
Ongoing communication with rheumatology teams
-
Diseases/Concerns Supported:
Crohn’s disease
Ulcerative colitis
Inflammatory bowel disease requiring infusion therapy
Care We Provide:
GI infusion therapy under physician-directed protocols
Referral accuracy review and medication verification
Required screening and lab review
Pre-treatment patient education
Monitoring of vitals, symptoms, and comfort during treatment
Documentation of response and infusion tolerance
Management of infusion reactions using standardized protocols
Coordination with gastroenterology offices for plan adjustments and reporting
-
Diseases/Concerns Supported:
Multiple sclerosis
Neuro-autoimmune conditions
Other neurologic conditions requiring infusion-based therapy
Care We Provide:
Neurologic infusion support under neurologist orders
Pre-infusion safety checks and medication verification
Symptom review before treatment
Vital signs and infusion tolerance monitoring
Observation for neurologic concerns during and after infusion
Protocol-driven rate adjustments
Reaction response support
Detailed documentation and communication with neurology teams
-
Diseases/Concerns Supported:
Immune deficiency disorders requiring IVIG
Provider-directed immunology infusion therapy needs
Care We Provide:
IVIG administration under provider orders
Weight-based dosing confirmation
Infusion rate titration per protocol
Hydration and pre-medication support as ordered
Close monitoring throughout treatment
Scheduled vital signs and response documentation
Escalation support for adverse reactions
Coordination with immunology teams on labs, scheduling, and post-infusion reporting
-
Diseases/Concerns Supported:
Autoimmune dermatologic conditions
Systemic inflammatory skin conditions requiring biologic therapy
Care We Provide:
Systemic biologic therapy support under provider orders
Medication verification and screening checklist review
Vitals monitoring during each visit
Protocol-driven infusion rate management
Documentation of treatment response and side effects
Structured updates to dermatology offices
Ongoing monitoring in a calm, patient-centered infusion environment
-
Diseases/Concerns Supported:
Iron deficiency anemia
Anemia requiring infusion-based treatment
Related hematologic support needs under physician orders
Care We Provide:
Iron infusion administration per physician orders
Medication verification and pre-infusion assessment
Vitals monitoring before, during, and after treatment
Patient education regarding therapy and expectations
Observation for infusion tolerance and adverse reactions
Documentation of patient response and progress
Communication with referring providers for follow-up needs
-
• Chronic inflammatory conditions requiring infusion-based therapy
• Patients requiring long-term biologic or immune-modulating medications -
Diseases/Concerns Supported:
Cancer treatment requiring infusion therapy
Solid tumor and hematologic oncology treatment support
Ongoing infusion-based cancer care under oncologist direction
Care We Provide:
Administration of prescribed oncology infusion therapies
Medication verification and treatment preparation
Pre-infusion patient assessment
Vital signs monitoring before, during, and after treatment
Close observation for infusion tolerance and side effects
Hazardous drug handling using proper safety protocols
Use of appropriate protective equipment and approved disposal methods
Clinical documentation of treatment response and patient status
Coordination and communication with the oncology care team
-
Diseases/Concerns Supported:
Cancer-related fatigue and weakness
Treatment-related side effects
Immune system support during oncology care
Supportive care needs during active cancer treatment
Care We Provide:
Administration of supportive infusion medications as ordered
Pre-treatment assessment and symptom review
Medication verification
Vital signs monitoring throughout the visit
Observation for tolerance and adverse reactions
Ongoing patient support during the infusion process
Documentation of symptoms, response, and supportive care needs
Coordination with the oncology team for continuity of care
-
Diseases/Concerns Supported:
Severe asthma
Chronic urticaria
Eosinophilic conditions
Other provider-directed allergy and pulmonary biologic therapy needs
Care We Provide:
Administration of biologic therapy as ordered
Pre-treatment screening
Medication verification
Review of relevant clinical history and labs
Patient education before treatment
Monitoring before, during, and after administration
Observation for adverse reactions
Use of established safety and escalation protocols
Clinical documentation of treatment response
Coordination with allergy, immunology, and pulmonary providers
Elena M., Patient
“From the moment we began working with this team, the level of care and coordination stood out. Every interaction felt thoughtful, organized, and highly professional. Appointments were handled seamlessly, communication was clear, and the clinical team demonstrated precision and attentiveness at every step. The environment, processes, and follow-through reflected a truly elevated standard of care. Knowing that my treatment was managed with this level of consistency and expertise gave me complete confidence and peace of mind.”

Follow Us on Social




Contact Us
Have a question, referral, or infusion placement to discuss? Alera Care provides premium, hospital-grade Specialty Infusion Services supporting rheumatology (RA, lupus, vasculitis), gastrointestinal care (Crohn’s, UC), neurology infusions (MS and neuro-autoimmune), immunology infusions (IVIG), dermatology infusion support (autoimmune biologics), and iron infusions with anemia management.
Our team coordinates closely with referring providers to help patients stay on schedule with safe protocols, attentive monitoring, and a calm, patient-first experience.
Call: 404-655-4637
Email: info@aleracaremedical.com
Web: www.aleracaremedical.com
